
9 years ago
5
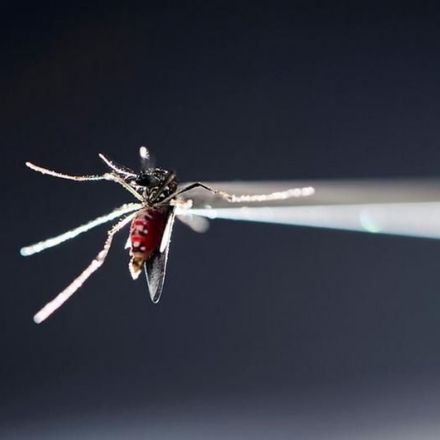
New malaria vaccine is fully effective in very small clinical trial
We may finally be getting somewhere in our fight against the disease.
Continue Reading
Additional Contributions:

























Join the Discussion
This is an exciting development, however, once again media is trying to make a sensation out of preliminary science. The vaccine prevented infection in 9 out of 9 (!!!!) volunteers ten weeks after the vaccination. Nine is an extremely small number of volunteers and this kind of trials primary tests the preliminary safety before larger trials. And while it gives hope, there's also a good chance that the vaccine will fail in a larger trial. Could be many things - with more testing, it could reveal toxicity, or lack of efficacy in larger groups of people, or it could stop working at week eleven after the vaccination. It's good to hear about the progress of science but let's not forget that science can be really tough and that there's many things that could go wrong before we actually have an effective malaria vaccine.
I was thinking about this and wondering about the ethics of conducting a large trial. It sounds like there would be considerable ethical issues. Even without a control group. Add a control group and how would that be ethically allowed?
What kind of ethical issues were you thinking about? I'm not an expert on organising clinical trials but here's how I think it could go: unless they need other smaller trials to check other things, the main task of the next trial would be confirming the efficacy of the vaccine while still keeping a close eye on the safety.
So they would have more participants and possibly a longer trial period. One group would receive the vaccine, the control group would receive an injection of saline (and wouldn't know that it's saline). Then, perhaps, the participants would just go about their lives and come back for check ups every now and then. The clinicians would then compare how many people get malaria in the control versus vaccinated group. For this they would use complicated statistical analysis to compare how many people get infected in each group.
Nobody would be infected on purpose, they would just try to see if any of the "real life infections" are prevented. And the control group would be no worse off than they would be without taking part in the trial.
The only downside of this approach? It would require a lot of participants and thus such trial would cost a lot. Also, it wouldn't give sensational headlines such as 100% efficacy ;)
Having a control group exposed to malaria without protection and actually getting malaria, I would think was an ethical issue.
Yes, it would. But in the scenario I described nobody gets infected on purpose and the exposure risk for control group is just as high as it would be without the trial. Does that make it ethically acceptable for you?